- Screening of all who enter the facility for signs and symptoms of COVID-19 (e.g., temperature checks, questions or observations about signs or symptoms), and denial of entry of those with signs or symptoms
- Hand hygiene (use of alcohol-based hand rub is preferred)
- Face covering or mask (covering mouth and nose)
- Social distancing at least six feet between persons
- Instructional signage throughout the facility and proper visitor education on COVID-19 signs and symptoms, infection control precautions, other applicable facility practices (e.g., use of face covering or mask, specified entries, exits and routes to designated areas, hand hygiene)
- Cleaning and disinfecting high frequency touched surfaces in the facility often, and designated visitation areas after each visit
- Appropriate staff use of Personal Protective Equipment (PPE)
- Effective cohorting of residents (e.g., separate areas dedicated COVID-19 care)
- Resident and staff testing conducted as required at 42 CFR 483.80(h) (see QSO-20- 38-NH)
Care Matters Spotlight October 2020
Mr. Borden admitted to Holzer Senior Care Center with the ultimate goal of returning home with his wife. Upon admission, Mr. Borden required the use of a feeding tube for nutrition and a mechanical lift to complete transfers. At first, returning home with his wife seemed like a lofty task due to the amount of assistance Mr. Borden needed. He soon became unmotivated and thought this goal was impossible due to apparently insurmountable tasks. Both he and his wife thought that he would be staying at the facility forever.
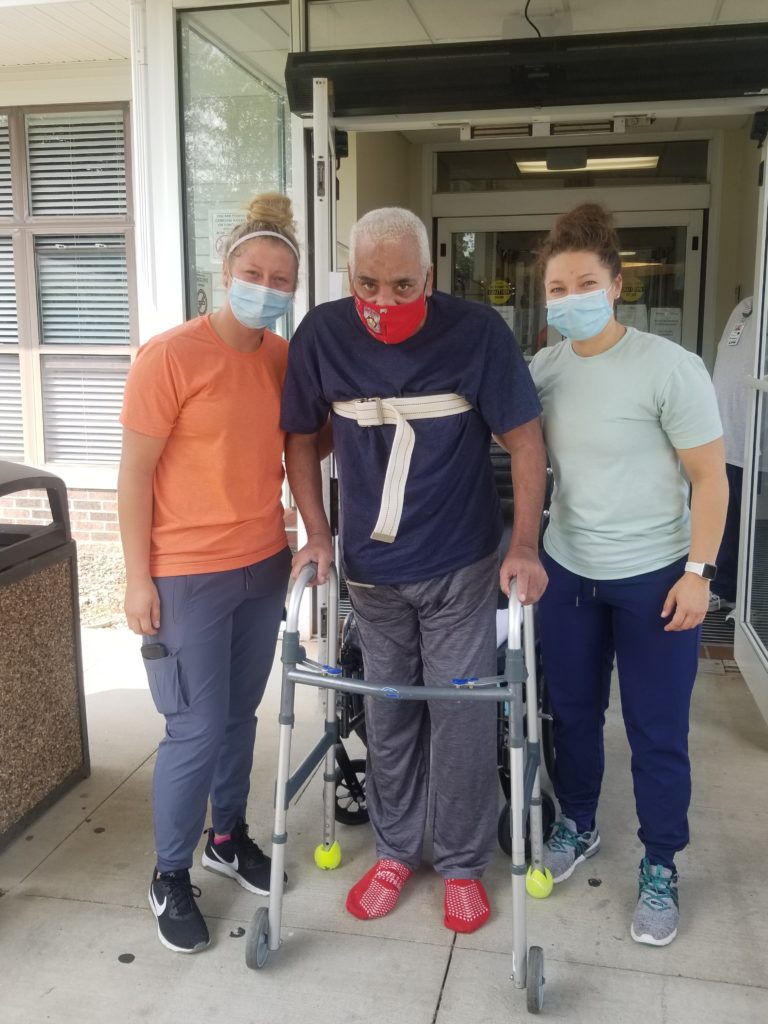
In the midst of this, Mr. Borden had a brief readmittance to the hospital and then returned to Holzer Senior Care Center with a new outlook and motivation. After putting his all into and excelling in an aggressive therapy program tailored to meet his needs, Mr. Borden began eating regular food and was able to walk out of Holzer Senior Care following his intensive program. What a great testament not only to Mr. Borden, but also to the excellent therapists and staff at Holzer Senior Care Center!
Mr. Borden’s ultimate goal was met; he was able to return home with his wife. Mr. Borden is pictured here, with his PT and OT, heading to embrace his wife after months of being separated from each other. The staff, Mr. Borden, and his wife had a “going home” parade and sang “O Happy Day” as Mr. Borden walked to the car. Needless to say, it was an emotional day for everyone as the Bordens hugged each other for the first time in 4 long months!
Great job Mr. Borden and awesome job, team!
Moving Forward: Safe and Successful Reintegration

In September, the Centers for Medicare and Medicaid Services (CMS) released exciting news for the advancement of safe visitation and resumption of group activities and communal dining in nursing homes (see QSO-20-39-NH). As the effects of isolation have taken a tremendous toll on our elderly population, care teams and residents are ready to implement safe steps to social reintegration. Facilities, including therapy departments, can now offer a variety of group activities while also taking the necessary precautions.
CMS provides Core Principles of COVID-19 Infection Prevention which should be incorporated as best practice to reduce the risk of COVID-19 transmission in order to resume visitation and group activities. It is indicated that group activities may be facilitated (for residents who have fully recovered from COVID-19 and for those not in isolation for observation, suspected or confirmed COVID-19 status) with social distancing among residents, appropriate hand hygiene, and use of cloth face coverings or facemasks. CMS’ examples of group activities include book clubs, crafts, movies, exercise and bingo.
As facilities implement these principles and activities, it is important to remember, early in the pandemic, resident-centered care plans were adapted for isolation considerations. These care plans should now be reviewed, especially in the light of infection control prevention, trauma-informed care, cognitive changes and fall prevention. It should not be assumed that residents will function at the same level as they did pre-pandemic; therefore, consider the increased risks associated with the possible secondary effects of the pandemic and isolation precautions:
- Infection Prevention and Control: Review the resident’s ability to safely wear cloth face coverings and understanding of or cueing needed for social distancing. Identify assistance and reminders needed to perform hand hygiene.
- Trauma-Informed Care (TIC): Consider whether the resident is suffering from anxiety associated with infection risk or recovery and provide a facility plan for safe reopening. Ensure staff buy-in to the plan and implementation in order to set good examples and provide TIC support. Be sensitive to the effects of a busy, potentially noisy, environment following a period of social isolation.
- Cognitive changes: As social interaction increases and the physical environment changes, be aware of behavioral responses and signs or symptoms of confusion. Assess behaviors as a form of communicative response to the environment and adapt as appropriate.
- Fall prevention: Consider that as the resident’s access to the facility and grounds expands, their environment is now exponentially larger. Review their ability to safely ambulate throughout the facility as this may place the resident at increased risk of falls and wayfinding confusion.
Protecting residents from COVID-19 highlights the struggle between keeping residents healthy and providing beneficial, daily experiences that can impact quality of life. Nursing, therapy, and facility staff must work as a team to implement creative means to facilitate safety during group activities and social reintegration to allow our residents to safely flourish in light of the challenges they encounter.
PHI Breaches and Breach Reporting
What is a breach of Protected Health Information (PHI)? A breach means the impermissible acquisition, access, use, or disclosure of PHI as defined under the Health Information Portability and Accountability Act (HIPAA) Privacy Rule that compromises the security or privacy of PHI.
Whenever a breach of PHI occurs, the residents impacted must be notified along with the secretary of the United States Department of Health and Human Services (HHS). Residents must be notified as soon as possible but no later than 60 days from discovery of the breach. This notification deadline to the Secretary of HHS varies depending on the number of residents impacted. If less than 500 residents are impacted, the deadline for notification to the Secretary is 60 days after the end of the calendar year in which the breach occurred. If 500 or more residents are impacted, the deadline for notification to the Secretary is no later than 60 days from the discovery of the breach.
Covered entities are required to report breaches to the Office of Civil Rights Breach reporting portal. The United States Department of Health and Human Services, in accordance with section 13402(e)(4) of the Health Information Technology for Economic and Clinical Health Act (HITECH), posts online a list of breaches impacting 500 or more individuals. This breach portal is unofficially labeled the “Wall of Shame”. CLICK HERE to visit the portal.
Interrupted Stay Policy
Under the Patient-Driven Payment Model (PDPM), there is a potential incentive for providers to discharge skilled nursing facility (SNF) patients from a covered Part A stay then readmit the patient in order to reset the variable per diem schedule. To mitigate this potential incentive, an interrupted stay policy is included within the PDPM.
This policy combines multiple SNF stays into one single episode in situations where the patient’s discharge and readmission occur within a prescribed window. If a patient is discharged from a SNF and readmitted to the same SNF no more than three consecutive calendar days after discharge, then the subsequent stay is considered a continuation of the previous stay. In this instance, the variable per diem schedule continues from the point just prior to discharge.
If the patient is discharged from a SNF and then readmitted more than three consecutive calendar days after discharge or admitted to a different SNF, then the subsequent stay is considered a new stay. In this instance, the variable per diem schedule resets to day one.
CLICK HERE for more information in the PEPPER User’s Guide Update.
CMS Memo on the Resident’s Right to Vote
The Centers for Medicare & Medicaid Services (CMS) released a memo reiterating the continued right of nursing home residents to exercise their right to vote. While the COVID-19 Public Health Emergency has resulted in limitations for visitors to enter the facility to assist residents, nursing homes must still ensure residents are able to exercise their Constitutional right to vote. A resident’s rights, including the right to vote, must not be impeded in any way by the nursing home staff.
Nursing home personnel should have a plan to ensure residents can exercise their right to vote, whether in person, by mail, absentee, or other authorized process. For residents who are otherwise unable to cast their ballots in person, nursing home staff must ensure residents have the right to receive and send their ballots via the U.S. Postal Service or other authorized mechanism allowed by the State or locality.
CLICK HERE to read the full memo from CMS.
Updated NHSN Pathway Reporting Mandatory for Point of Care Testing in Skilled Nursing Facilities
The Centers for Disease Control & Prevention (CDC) and the Centers for Medicare & Medicaid Services (CMS) are now requiring nursing facilities to utilize the CDC’s National Healthcare Safety Network (NHSN) as the required reporting pathway for the COVID -19 testing results that nursing facilities are generating from point of care (POC) testing devices which were provided by the Department of Health & Human Services (HHS).
Data collected via NHSN is pushed to the AIMS platform, which is hosted by the Association of Public Health Laboratories, every two hours. The AIMS platform then shares this data with state and local health departments as well as with HHS.
Currently, entry of data into NHSN is manual and entered one patient at a time. The CDC indicated that it plans to make accepting a CSV file, for multiple persons and test results at one time, possible in the future.
CLICK HERE for more information from HHS on reporting requirements.
Incentive Payments to Nursing Homes Curbing COVID-19
The U.S. Department of Health and Human Services (HHS) announced it will distribute approximately $333 million in first-round performance payments to over 10,000 nursing homes. These nursing homes are being recognized for demonstrating significant reductions in COVID-19 related infections and deaths between August and September.
Nursing Home Performance-Based Results
HHS announced that in the first round of the incentive program, 10,631 of the 13,795 eligible nursing homes met the infection control criteria. Overall, these nursing homes contributed to 5,000 fewer COVID-19 infections in nursing homes in September than there were in August. Against both the infection control and mortality criteria, 10,501 nursing homes qualified for payments and contributed to 1,200 fewer COVID-19 related nursing home deaths between August and September.
Nursing homes will receive September quality incentive payments next week and will have four more opportunities to receive additional incentive payments.
CLICK HERE for a state-by-state breakdown on incentive payments from this first cycle.
CLICK HERE for more information on the Provider Relief Program.
CLICK HERE to read the full press release from HHS.
HHS Provides Update for Provider Relief Fund Reporting Requirements
On Oct. 22, The Department of Health and Human Services (HHS) released a memo stating that they are no longer limiting providers’ use of Provider Relief Funds for covering lost revenue due to the coronavirus. HHS announced that it will go back to allowing providers to calculate their lost revenue based on the difference between their 2019 and 2020 actual patient- care revenue, and eliminate limits on how much Provider Relief Fund (PRF) payments can be applied to that lost revenue.
HHS added that the amended reporting instructions should allow providers to fully apply PRF distributions to lost revenues.
CLICK HERE to read the full memo.
Deadline to Sign Up for Vaccine Program Extended
On Oct. 16, the U.S. Department of Health and Human Services (HHS) and Department of Defense (DOD) began offering sign-ups for agreements with CVS and Walgreens to provide and administer COVID-19 vaccines to residents of long-term care facilities (LTCF) nationwide with no out-of-pocket costs. LTCF residents are anticipated to be part of the prioritized groups for initial COVID-19 vaccination efforts until there are enough doses available for every American who wishes to be vaccinated.
LTCFs will now have UNTIL NOVEMBER 6 to opt in and indicate which pharmacy partner their facility prefers to have on-site. LTCFs are not mandated to participate in this program and can request to use their current pharmacy contracts to support COVID-19 vaccination.
Nursing homes can sign up via the National Healthcare Safety Network (NHSN) and assisted living facilities can sign up via an online survey.
The CDC is offering an overview and FAQs, updated as of 10/23/20, to help further explain the program and AHCA/NCAL also are offering an overview.
CMS Updates Methodology for Calculating COVID-19 Testing by Nursing Facilities
The Centers for Medicare & Medicaid Services (CMS) announced a change in its methodology for calculating county-level community infection rates for COVID-19. Facilities are expected to use the county-level color coded rating (green, yellow, or red) to determine the frequency for testing facility staff and residents in accordance with CMS guidance.
The earlier guidance and methodology required facilities to test staff once monthly if the county in which the facility is located had a positivity rate of less than five percent (< 5%); testing frequency increased to once each week for county positivity rates between five and 10 percent (5 – 10%) and twice weekly for county positivity rates that exceeded 10 percent (>10%). The shift in methodology will mean a change in the color-coding rates. For example, CMS’ new methodology classifies counties with both fewer than 500 tests and fewer than 2,000 tests per 100,000 residents, along with a positivity rate greater than 10 percent over 14 days as “yellow” whereas the earlier methodology would have put these counties in the red zone.
CLICK HERE to read CMS’ press release about the change in methodology.
CLICK HERE for the latest county positivity rates.
CMS Posts Updated PDPM Grouper
The Centers for Medicare & Medicaid Services (CMS) posted an updated PDPM Grouper DLL v1.0007 to the MDS 3.0 Technical Information webpage.
CMS indicates that six ICD-10 codes were “inadvertently excluded from the NTA calculation.” The ICD-10 codes include: T8484XA, T8389XA, T8321XA, T82399A, T82392A and T83021A.
The PDPM Grouper DLL v1.0007 package notes that PDPM can be used for OBRA assessments where A0310A =[01,02,03,04,05,06] and A0310B = [99] as determined by each state. CMS also notes that FY2021 ICD-10 codes must be used for I0020B in these assessments as well as for the I8000A-J items in MDS assessments with a target date on or after October 1, 2020.
CLICK HERE to access the zip file.
CMS Changes Medicare Payment to Support Faster COVID-19 Diagnostic Testing
The Centers for Medicare & Medicaid Services (CMS) announced new actions to pay for expedited COVID-19 test results. CMS announced that starting January 1, 2021, Medicare will pay $100 only to laboratories that complete COVID-19 diagnostic tests within two calendar days of the specimen being collected.
Also, effective January 1, 2021, for laboratories that take longer than two days to complete these tests, Medicare will pay a rate of $75. CMS reports they are working to ensure that patients who test positive for the virus are alerted quickly so they can self-isolate and receive medical treatment.
CLICK HERE to review the full press release from CMS.
CMS Announces New Repayment Terms for Medicare Loans Made to Providers During COVID-19
The Centers for Medicare & Medicaid Services (CMS) announced amended terms for payments issued under the Accelerated and Advance Payment (AAP) Program. Under the Continuing Appropriations Act, 2021 and Other Extensions Act, repayment will now begin one year from the issuance date of each provider or supplier’s accelerated or advance payment.
Providers were required to make payments starting in August of this year, but repayment will be delayed until one year after payment was issued. After that first year, Medicare will automatically recoup 25 percent of Medicare payments otherwise owed to the provider or supplier for eleven months. At the end of the eleven-month period, recoupment will increase to 50 percent for another six months. If the provider or supplier is unable to repay the total amount of the AAP during this time-period (a total of 29 months), CMS will issue letters requiring repayment of any outstanding balance, subject to an interest rate of four percent.
Guidance is also provided on how to request an Extended Repayment Schedule (ERS) for providers and suppliers who are experiencing financial hardships. An ERS is a debt installment payment plan that allows a provider or supplier to pay debts over the course of three years or up to five years in the case of extreme hardship. Providers and suppliers are encouraged to contact their Medicare Administrative Contractor (MAC) for information on how to request an ERS.
CLICK HERE to read the full press release from CMS.
Speech Language Pathology’s Role in COVID Recovery
The novel coronavirus and resulting pandemic have altered our lives in many ways. The combination of isolation, physical and social distancing, as well as an economic crisis have all impacted our personal and professional lives. Juggling the ever-changing responsibilities during a healthcare emergency may be overwhelming. The lack of social connections with family and friends as well as in-person visits with your patients can lead clinicians to feelings of loneliness and isolation. Now consider the impact that continued social distancing and isolation may have on the residents and patients within our long-term care facilities. In some instances, isolation of residents has been ongoing for the entirety of the pandemic, entering nearly 6 months!
Prior to this healthcare emergency, a 2019 University of Michigan study on healthy aging noted that 34% of adults aged 50-80 years reported feeling lonely. This current period of social isolation will only exacerbate the number of adults feeling disconnected and lonely and disproportionately affect the elderly population, especially those whose primary social contacts were within their long-term care facility. Furthermore, according to the National Academics of Sciences, Engineering, and Medicine, “Seniors who are experiencing social isolation or loneliness may face a higher risk for mortality, heart disease, and depression.”
As experts on communication, SLPs know the value and need for social interaction for the mental health and well-being of our patients. We are a major factor in the identification of patient needs and educating patients and caregivers on appropriate and personalized techniques to improve and maintain cognitive, speech-language, and executive functioning. We can start by educating on the importance of social interaction and modeling how to achieve this safely during the pandemic.
In the absence of cognitive stimulation and routine, patients may have trouble maintaining prior levels of cognition. We can encourage and educate on the use of daily orientation techniques and maintaining daily routines – targeting problem solving, reasoning, memory, and sequencing during morning and evening self-care routines. Engage with each patient on a personal level and encourage all caregivers to do the same. Provide insight to caregivers on personal preferences that may enhance engagement.
Socialization and purpose play a critical role in feelings of self-worth and success in everyday life. Encourage the use of personal electronic devices. Provide education on increasing socialization through communication and social media. Encourage residents to write letters to family or “neighbors” within the facility. Foster conversation between residents and caregivers during meals and invite family or friends to “dine” with residents via videoconferencing.
Incorporate training on personalized “home” exercise programs to give purpose and focus to each resident’s day. Develop exercises that capitalize on the routines the resident has already established, such as oral motor exercises and/or breathing exercises during a TV commercial break.
As we evolve as professionals during a pandemic, we must continue to protect and advocate for our most vulnerable residents. With the continuation of the healthcare emergency there is a fine line between protecting those that are medically fragile from this virus while continuing to encourage and promote socialization that is vital to their well-being. As visitor restrictions are lessened we continue to be the lifeline that can bring awareness to the effects of social isolation on our residents in long-term care, and by supporting the facility and promoting each caregivers’ strengths as well as educating in areas of opportunity we are creating a more understanding and supportive environment for our residents.
https://time.com/5833681/loneliness-covid-19/
Occupational Therapy’s Role in COVID Recovery
As we all have become acutely aware of, COVID-19 and the response to the pandemic have resulted in adverse outcomes to residents of skilled nursing and long-term care facilities. These adverse outcomes range from reduced physical function, including decreased muscle strength and endurance, to cognitive and psychosocial impairments, including delirium, neurological dysfunction, depression, and occupational deprivation. In combination, these symptoms paint a clear picture for the need of occupational therapy (OT) intervention. As OT practitioners, we must identify and champion our unique role in not only the physical rehabilitation of our patients but also in their psychological well-being.
According to the American Journal of Occupational Therapy’s (AJOT) OT Practice Framework, our profession, in its fullest sense, is facilitating achieved “health, well-being, and participation in life through engagement in occupation.” We identify the areas of occupation that our residents value, consider their context, and recognize the unique performance patterns and skills that affect the individual’s ability to engage and participate. This is clearly a client-centered, holistic process—one that considers physical function, cognition, and psychosocial impairments that may be impacted. Who better to address the wide range of outcomes that have resulted with our residents in skilled nursing and long-term care facilities?
As we continue to care for our residents who have been affected directly or indirectly by COVID-19, it is imperative that we implement this client-centered, holistic approach. How has the individual’s physical function been affected? Consider implementation of a cardiopulmonary program that includes respiratory strategies, postural control exercises, and exercise prescriptions. To address changes in cognition, complete a standardized cognitive assessment to identify specific processing skills for intervention during activities of daily living. Equally important, and even more important in some cases, are the psychosocial challenges that residents face during the pandemic. As patients are isolated to reduce transmission risks, unintended negative consequences present, including disruption of daily routines and restrictions to leisure and social participation. Recent studies suggest that isolation- associated loneliness has contributed to swift health declines in residents with dementia during the COVID-19 pandemic. Recognize and affirm residents in the challenges they face and use creative technological outlets to enhance participation in meaningful daily activities. Are there opportunities for virtual conferencing with friends or family? Are audio books, online games, or learning modules an option for leisure?
As OT practitioners, we are equipped to meet the tidal wave of challenges that COVID-19 has introduced to residents in skilled nursing and long-term care facilities. The tenets of our profession prepare us to respond to the physical, cognitive, and psychosocial changes that may occur. Though relaxed restrictions to nursing home visitation are on the horizon, the time is now to take hold of our unique, distinct role in facilitating health, well-being and participation in the lives of our residents.
References:
American Occupational Therapy Association. (in press). Occupational therapy practice framework:
Domain and process (4th ed.). American Journal of Occupational Therapy, 74 (Supplement 2). Advance online publication.
De Biase, S., Cook, L., Skelton, D. A., Witham, M., & Ten Hove, R. (2020). The COVID-19 rehabilitation
pandemic1. Age and ageing, 49(5), 696–700. https://doi.org/10.1093/ageing/afaa118
Gitlow, L., PhD, ATP, FAOTA, OTR/L, Lee, S., OTR/L, Hemraj, R., OTR/L, Sheehan, L., OTD, OTR/L, & Ambroze, G., OTS. (2020). Occupational Therapy and Older Adults: Combating Social Isolation through Technology. PDF. American Occupational Therapy Association.
Lasek, A. (2020, September 18). Dementia mortality skyrockets since lockdowns; CMS loosens visitor restrictions – Clinical Daily News. Retrieved September 18, 2020, from https://www.mcknights.com/news/clinical-news/dementia-mortality-skyrockets-since-lockdowns-cms-loosens-visitor-restrictions/?utm_source=newsletter
Physical Therapy’s Role in COVID Recovery
For over 100 years, physical therapists have specialized in human movement using skilled interventions to maximize health and function. During periods of critical illness, such as moderate to severe cases of COVID-19, it is common for patients to experience a loss of physical function which can lead to the development of new impairments or worsening of existing ones.
Long-term recovery from COVID-19 may be complicated by lasting effects due to deconditioning, restrictive lung disease, post intensive care syndrome, or neurological disorders. After 10 days of bed rest healthy older adults may lose up to 2.2 pounds of muscle mass from the legs with 2-5%/day loss of muscle strength. Recovery of physical function may take an extended period of time with impairments that may persist up to 2 years post infection.
As practitioners of movement, physical therapists are essential in early mobility during and following a critical illness in order to minimize the effects of immobility. Through skilled interventions such as functional mobility, balance training, endurance activities, posture training, and strengthening, physical therapists are equipped to help residents achieve their optimal level of function as quickly and effectively as possible.
Along with debility, residents in nursing homes that remain quarantined during the public health emergency face another silent threat: social isolation. Even with the recent relaxation of nursing home visitor guidelines, the effects of social isolation may be long lasting.
Restricted access to family and friends may affect even those who have not contracted the virus itself and may include severe fatigue, anxiety, post-traumatic stress disorder, depression, and cognitive dysfunction.
The effects of patients remaining in their room, the cessation of communal dining, and restricted access to common areas (i.e. the therapy gym and equipment) pose significant barriers not only to successful intervention and outcomes, but also overall resident well-being. The interdisciplinary team should assess and re-assess situations, analyze tasks, make changes, and consider a holistic plan of care to help reduce the lasting effects of social isolation and provide person-centered, specialized care which emulates Reliant’s motto of Care Matters.
References:
https://www.bsrm.org.uk/downloads/covid-19bsrmissue1-published-27-4-2020.pdf.
https://academic.oup.com/ptj/article/100/9/1458/5862054
https://www.aannet.org/initiatives/choosing-wisely/immobility-ambulation
Breast Cancer Awareness Month Activities
Most people know someone who has been diagnosed with breast cancer. This month, we remember those brave individuals we’ve lost and send lots of healing thoughts to those who still are fighting. Here are some ways you can foster a community of support to those women—and men—and their families.
Pink Pumpkins Why not!?
Organize a simple activity to have residents, patients, employees and family members paint or decorate mini-pumpkins in pink to spread awareness—and cheer—throughout residential and therapy areas.
Wear Pink
Raise awareness in the community by asking everyone to wear pink for a day or a week to remember, support and advocate for breast cancer awareness.
Host a Support Group
Work with a local oncologist and host a support group or event for women battling breast cancer to connect with each other, share their stories and offer support.
Hold a Hat & Scarf Drive
Collect or make hats or scarves to donate for women who are going through chemotherapy at a local center.
Support Prevention Programs
Host an information session with one of the community nurses, physicians or nurse practitioners to talk about how to do self exams and the importance of regular mammograms to catch breast cancer early enough for effective treatment.
Aging and Mammography
We’re living longer than ever. The median life expectancy for an 80 year old woman is nine years, so if you’re generally healthy, it can make sense to continue screening through the 70s and perhaps early 80s. As the American Cancer Society recommends, “Women should continue screening mammography as long as their overall health is good and they have a life expectancy of 10 years or longer.”


